Chorioretinopathy associated with trauma or systemic injury, characterized by cotton lint spots, retinal hemorrhage, optic nerve edema and retinal ischemia, is called purtschers retinopathy, which is a very rare clinical disease. The vitreoretinal macular expert from Milburn, New Jersey, reported a rare case of monocular vision loss in a pregnant woman with preeclampsia, sharing the disease characteristics and diagnosis and treatment process.
Extremely rare purtschers retinopathy
In 1910, Otmar purtscher published an article describing a patient with bilateral visual loss after head trauma. The examination found that the patient had bilateral retinal hemorrhage and whitening. This chorioretinopathy, which is related to trauma or systemic injury, is characterized by lint spots, retinal hemorrhage, optic nerve edema and retinal ischemia, and is called purtschers retinopathy.
The causes of the disease include pancreatitis, fat embolism, air embolism, amniotic fluid embolism, HELLP syndrome, trauma, long bone fracture, preeclampsia and eclampsia.
Purtschers retinopathy is extremely rare despite its diverse etiology. A study found that in Britain and Ireland, the incidence rate was 0.24 per million people. In the latest case report, a pregnant woman with preeclampsia experienced acute unilateral visual loss secondary to purtschers retinopathy. Clinicians searched the literature of "purtscher retinopathy in preeclampsia" with PubMed and Scopus, and found no other cases of unilateral visual involvement and purtscher retinopathy in preeclampsia patients.
Pregnant women's visual acuity drops suddenly, which is actually caused by purtschers' retinopathy
A 23-year-old black woman was 27 weeks pregnant, her right eye vision decreased for 3 days, and she had obvious anemia in her previous history. Check that BVCA is 20/250 OD, 20/20 OS. There was no significant change in anterior segment examination and intraocular pressure. In the funduscopy, the change of the left eye was not obvious, and the funduscopy of the right eye showed venous dilatation with scattered flame like bleeding, cotton wool spots and purtscher spots around the lower nipple (Fig. 1). OCT showed retinal thickening, subretinal effusion and edema of nerve fiber layer (Fig. 2). The blood pressure was 174/122 due to delayed fluorescein angiography during pregnancy. In view of these findings, doctors diagnosed purtschers retinopathy and speculated that it might be caused by preeclampsia.
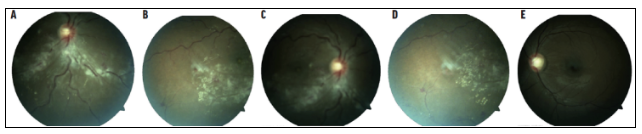
Figure 1 Fundus imaging of the right eye showed venous dilatation (a), cotton spots (b), hemorrhage (c) and purtscher spots (d); Left eye unaffected (E)
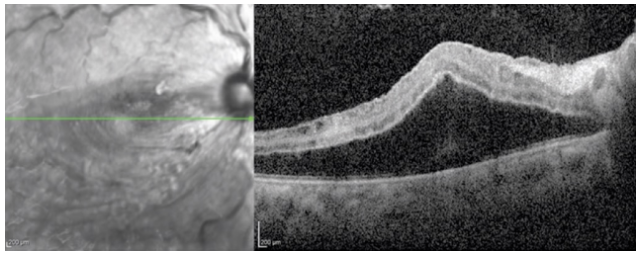
Figure 2 OCT showed retinal thickening, macular edema, subretinal effusion and edema of nerve fiber layer
Due to the presumed diagnosis of preeclampsia, the patient was urgently transferred to obstetrics. The patient did not follow up as recommended by the doctor, and went to the emergency department one week later. The examination results showed that: the blood pressure was 168/94, proteinuria was 4+, and the diagnosis was preeclampsia; Two days later, caesarean section was performed and two healthy infants were born. At 11 weeks after delivery, VA in the patient's right eye was the index, and fundus examination showed that:
The optic nerve was pale, the diameter of retinal vessels returned to normal, and subretinal effusion and macular edema almost disappeared.
Fluorescein angiography showed that the infratemporal and peripheral non perfusion areas were wedge-shaped, the brightness decreased, and the perfusion time was normal (Fig. 3).
Fine lace collateral vessels can be seen near the non perfusion area, and there is no late leakage in the center.
The findings of this patient are consistent with inflammatory optic atrophy and retinal ischemia sequelae caused by purtschers retinopathy. So far, VA in the patient's right eye is still an index.
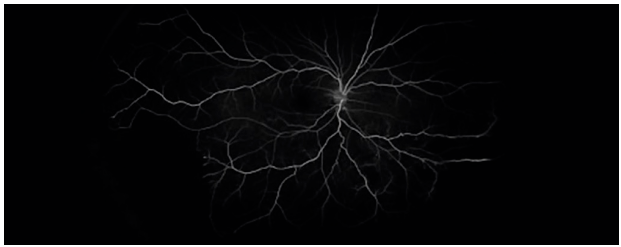
Figure 3 Fluorescein angiography showed low fluorescence in the wedge-shaped area
Presentation and treatment of purtschers' retinopathy
Purtschers' retinopathy is a small arterial microvascular disease characterized by the supply of superficial retinal capillaries with a diameter of 45 μ The small arteries around the nipple are occluded, and patients usually show acute visual loss. The common results of ophthalmoscopy were cotton lint spot (93%), retinal hemorrhage (65%) and purtschers spot (63%). Purtschers retinopathy should be suspected in cases with the above three signs.
One study recorded data from patients with purtschers' retinopathy (24 eyes) at 1 month and 6 months. At 1 month, 74% of the eyes still had acute retinopathy, such as bleeding, lint spots or purtscher spots; At 6 months, 100% of acute retinopathy disappeared; In addition, the visual acuity of 50% eyes improved by 2 lines, and that of 23% eyes improved by 4 lines, an average of 2.7 lines. The final visual acuity of 11 of 24 eyes was 20/200.
Another study found that 10 of the 25 patients had a VA value of 20/200 or less in at least one eye in the final visual acuity assessment.
The treatment of purtschers' retinopathy is usually limited to the treatment of basic diseases (in this case report, it is preeclampsia pregnancy), waiting for symptom relief. Previous case reports showed that the use of 250mg intravenous glucocorticoid for 3 days, 4 times a day, could improve vision. The mechanism of high-dose glucocorticoids to improve prognosis is to stabilize the damaged neuronal cell membrane. A case report describes in detail a patient with purtschers' retinopathy whose visual acuity improved from 20/800 to 20/50 after 1 week of glucocorticoid therapy.
In the above cases, the unilateral involvement of the patient may be the result of the anatomical difference between the small arteries of the left eye and the right eye. Blood flow studies suggest that retinopathy may be the result of the interaction between vascular branches, blood flow volume, capillary wall stress, endothelin peptide, procycline, nitric oxide levels and local self-regulation. The increase of blood flow velocity caused by hypertension induced by preeclampsia may lead to the change of vascular wall stress. The difference of microvascular bifurcation angle between the left and right eyes may lead to different degrees of wall stress, resulting in unilateral involvement.
Delayed diagnosis and intervention of preeclampsia may lead to permanent damage of end organs including eyes. This case highlights the need for aggressive treatment of these patients, usually by accelerating delivery to improve patient outcomes. In the absence of effective treatment for acute occlusive retinal vascular disease, prevention through vigilance and management of systemic risk factors is the best and feasible way to reduce visual loss.
reference material: https://retinatoday.com/articles/2022-jan-feb/an-unusual-case-of-unilateral-purtschers-retinopathy